From Death Sentence to Debt Sentence
Finance & Development, December 2015, Vol. 52, No. 4
Paul Collier, Richard Manning, and Olivier Sterck

Now that AIDS is a controllable disease, countries and donors must focus on financing treatment and investing in prevention
TWENTY years ago, a diagnosis of AIDS meant certain death. Now, thanks to antiretroviral therapies, people living with the HIV virus in low-income countries can enjoy a near-normal life at a cost of a few hundred dollars a year. Initially, it was thought that these therapies might not be viable in Africa given the difficulty of adhering to the demanding routine of treatment (Stevens, Kaye, and Corrah, 2004). But these fears have proved groundless: millions of Africans are alive and healthy today thanks to such therapies.
Reflecting this perception that the medical battle against AIDS is now winnable, an Economist cover story marking the 30th anniversary of the disease was titled “The End of AIDS?” But as the end of AIDS as a medical disaster comes within reach, it has become a potential fiscal calamity. Vastly improved survival rates for people who are HIV positive mean that poor countries with high HIV prevalence face a major new fiscal liability (Haacker and Lule, 2011).
Moral dilemma
The HIV virus gradually destroys white blood cells, essential to the operation of a person’s immune system. Without treatment, people whose CD4 count—a measure of these white blood cells—falls below 350 cells/cubic millimeter are likely to die within five years; with treatment they can live nearly normal lives. Despite the availability of generic and discounted drugs in poor countries, the cost of treatment is too high for sufferers who are poor—and too high for poor societies to bear on their behalf. But from the perspective of high-income countries this cost is trivial—a few hundred dollars to save a life. These features give rise to an obligation of rescue: identifiable HIV-positive people cannot be left to die when it is so readily in our power to prevent it. That is why past leaders, such as U.S. President George W. Bush and French President Jacques Chirac, who did not regard development aid as a high priority, nevertheless launched massive and dedicated funding for HIV/AIDS programs.
But the cost of financing antiretroviral treatment poses its own unique moral issues. Once treatment is started, it would be abhorrent to stop it because funds run out. Choosing to discontinue treatment is an “act of commission” that ends the lives of identifiable people rather than the “act of omission” of failing to start treatment. But expenditures on antiretroviral treatment are long lasting precisely because treatment enables normal life spans: currently young sufferers will have to be treated for decades.
Thanks to antiretroviral therapies and prevention, the number of people who are newly infected with HIV is declining in most parts of the world. Between 2001 and 2013, the number of new HIV infections declined by 38 percent, from 3.4 million to 2.1 million (UNAIDS, 2014). AIDS-related deaths have also fallen thanks to treatment, by 35 percent since 2005. However, since the number of new infections in many countries is still well above the number of deaths, the stock of HIV-positive citizens continues to increase, meaning that the costs are likely to escalate for many years. In addition, most of the people already infected with HIV are not yet on antiretroviral therapy, either because their CD4 count has not yet fallen to the point at which treatment is warranted or because they have not yet been diagnosed. So many more people will at some stage need treatment. And worse, many of the people receiving therapy—and those who will need it in the future—will eventually become resistant to the standard treatment. At that point they will need more sophisticated treatment regimens, which are considerably more expensive.
The distinctive features of these costs have two potent implications that justify our focus on HIV/AIDS. However, our framework can be adapted to study the implications of other health conditions with the same features, and our analysis is of course not intended to minimize the requirement for investment in other health needs.
First, because the decision to start treatment locks in the need to finance future provision, that future liability needs to be known in advance. Donors and the governments of affected countries then must agree on clear rules for how that cost will be shared. Otherwise, governments might reasonably be wary of incurring liabilities that would not be viable if donor attention shifts to other priorities.
Second, because the continuing spread of infection creates large future liabilities, there is a new rationale for prevention policies. While no longer medically essential to prevent death, prevention becomes more financially valuable. It is worth expanding spending on prevention at least until an extra dollar averts a dollar of liability from new infections.
This means that the treatment and prevention of HIV/AIDS shifts from an issue concerning ministers of health to one that also directly affects ministers of finance. New research suggests that committing additional resources to HIV prevention could save a country money overall (see Collier, Sterck, and Manning, 2015, and related papers from the RethinkHIV consortium).
Counting the costs
In our research, we examined the prevalence of HIV and its future fiscal implications for eight African countries. We recognize that there are clear benefits to treating HIV/AIDS in terms of individual well-being and the economy, but our focus here is on the fiscal implications of the moral duty to rescue (see table). We use a standard epidemiological model integrated in the widely used Spectrum software to estimate the likely spread of infections until 2050 (Avenir Health, 2014). Then we calculate the total cost of future treatment. The unit costs come from Schwartländer and others (2011) and are assumed to be constant over time. We reduce future costs by the “discount rate,” which is the rate of interest. The higher the rate of interest, the lower the value of the liability today of costs that occur in the future. Generally, health economists use an interest rate of only 3 percent, which would imply a massive liability. In our work we use the higher (and therefore more conservative) rate of 7 percent—the rate at which African governments can currently borrow in sovereign debt markets—since this is a clearer reflection of opportunity costs. Even with this high discount of future expenditures, the liabilities arising from the treatment of HIV/AIDS are large enough to have an impact on countries’ economies.
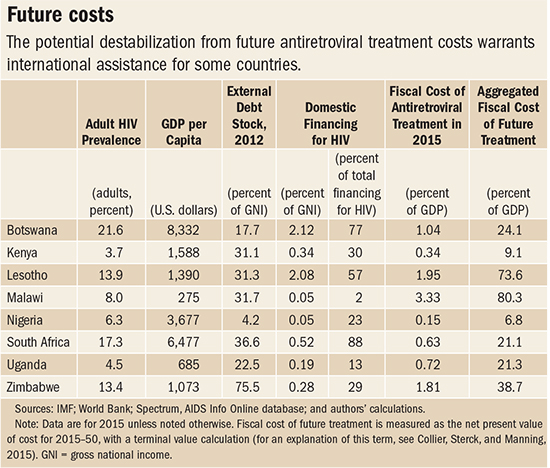
More than 10 percent of the population in four of the eight countries we studied—Botswana, South Africa, Zimbabwe and Lesotho—has the disease.
Taking into account the continuing spread of HIV, both Botswana and South Africa face a liability of over 20 percent of GDP arising from the need for treatment. Because both are middle-income countries, they cannot count on the international community to shoulder much of this future burden. Fortunately, because both countries have been prudently managed and therefore have low or moderate overall levels of debt to GDP, the treatment liability is substantial but not destabilizing. In fact, the response against HIV is already largely financed domestically in Botswana and South Africa.
Zimbabwe has a somewhat lower prevalence of the disease than Botswana or South Africa, but a much lower income level and a higher recognized debt burden. In this case, it would be desirable to agree in advance on burden sharing with potential donors. Otherwise, there is a danger of a game of chicken between donors and government, each underfunding so as to leave the other with the duty of rescue.
Lesotho is in an altogether different situation. It is much poorer than Botswana or South Africa, but has a similar level of HIV infection. As a result, it faces a dramatically larger liability, analogous to a debt in excess of 70 percent of GDP. Lesotho’s external debt is only 31 percent of GDP, but the HIV-related liability would raise the country’s overall burden above 100 percent, in effect thrusting it into a debt level defined by the IMF’s Heavily Indebted Poor Countries Initiative as unsustainable. For this very reason, donors should not leave Lesotho to face this burden on its own. The international community already recognizes that external unsustainable debt burdens of poor countries should be forgiven. Lesotho has a small population, so the financial burden on the international community of financing the country’s HIV/AIDS expenses will be trivial.
In Malawi, despite the lower HIV prevalence, the cost burden of future treatment dwarfs the country’s modest external indebtedness. But because Malawi is much larger than Lesotho, the costs to the international community will necessarily be much higher. The Malawian government must therefore have reasonable reassurance of future donor funding if it is to commit to future treatment.
Clearly, given these liabilities for future treatment, ministries of finance must be aware of HIV/AIDS, and consider how to minimize the implied risks. Even for Uganda, which has lower prevalence, the hidden liability of treatment is as large as recognized indebtedness.
For some of the countries we studied, liabilities far exceed the capacity of the government to bear them. Given that there is an obligation of rescue, the excess of liabilities for treatment over what a country can reasonably afford becomes a liability of the donor community, and funding it will stretch for decades into the future. Ministries of finance must pressure donors to clarify their future commitments. Although donors face constraints on their ability to make long-term commitments legally binding, an agreed burden-sharing framework would make it less likely that donors will divert funds in the future to newly fashionable priorities.
The special funds that the international community has built to tackle HIV/AIDS have been crisis responses to the new duty of rescue, with short-term funding horizons rather than long-term strategies of partnership with African governments. But the likely evolution of each country’s funding requirements can be projected through analysis of historical government and donor spending on HIV/AIDS. For a given HIV prevalence, as per capita income rises, government spending increases too. But donor spending declines almost dollar for dollar with higher government spending, so that total spending on HIV/AIDS stays roughly constant. Unless ministers of finance can successfully renegotiate this pattern of burden sharing, they will have to accept that as their economies grow, escalating treatment costs will increasingly fall on their own budgets.
Countries that decide on renegotiation can draw on some existing benchmarks that could trigger relief—for example, the point at which a country’s total burden of future liability of antiretroviral treatment plus recognized external indebtedness exceeds the agreed debt sustainability threshold. Building an international consensus for such renegotiation would of course be no light task.
Whatever is done, donors and governments should not sleepwalk into a future crisis in which millions of people face the imminent prospect of avoidable death while each party tries to pin responsibility on the other. That said, spending money and providing drugs alone are not likely sufficient to defeat HIV; continuous investments to increase testing rates, diffuse knowledge, and promote prevention are essential.
An ounce of prevention

Our estimates of the cost of the duty of rescue underscore the need for effective policies to prevent the spread of infection. For Lesotho and Uganda, about half the future fiscal liability comes from new infections. And for Malawi, new infections increase the liability from 50 percent to 80 percent of GDP. On medical grounds, since the discovery of antiretroviral therapy, expanding treatment has taken precedence over prevention, but now there is a powerful fiscal rationale for greater attention to curtailing the spread of infection.
The initial policy response by the international community has been to promote treatment as the key to prevention. Once people are on antiretroviral therapy, they are far less infectious. The World Health Organization (WHO, 2015) is currently using this as one argument for treating people long before it is necessary to avoid death. However, this extension to treatment-as-prevention would be a further massive fiscal commitment, and in terms of the prevention objective other means of reducing the spread may be more cost-effective.
For example, in simulations for Malawi, we find that while the expansion of an adult circumcision program would more than pay for itself in reduced fiscal liabilities, an expansion of treatment-as-prevention would not. Good progress has been made by African countries in some areas, such as prevention of mother-to-child transmission. Encouraging adolescent girls to stay in school has also shown promising results (Santelli and others, 2015), but currently there are not enough proven prevention programs. Rather than pouring huge sums into the further expansion of treatment-as-prevention, it may be better to pilot a range of other prevention strategies, including those designed to achieve changes in sexual behavior, to see which work best.
The fear of inadvertently stigmatizing those who are HIV positive has often inhibited nonmedical approaches to policy. An early straightforward campaign of Ugandan President Yoweri Museveni, which warned people of the risks of multiple partners, proved to be highly effective. Ugandan infection rates subsequently rose again when the first campaign was replaced by a less realistic one advocating sexual abstinence. Similarly, there is a good case for intensively targeting sex workers and truck drivers—key groups spreading infection—for preemptive treatment. More precise geographic targeting would also make sense: for example, in Kenya risks of infection can vary tenfold between one county and the next.
A final important implication of our results is that donors and governments should closely align the share that each takes of the costs of treating future infections and of the costs of prevention. Any significant departure from this principle would expose the parties to moral hazard. For example, if donors paid for most of the treatment of future infections but governments paid for most of the prevention (or vice versa), neither party would have a financial incentive to increase spending on prevention to its cost-effective level. Despite the many billions of dollars spent to date on HIV/AIDS, this basic principle of incentive-compatible financing has not been recognized, let alone implemented. The principle will become much more important as effective prevention strategies are discovered and need to be scaled up.
To date, governments have left HIV/AIDS issues largely to ministries of health, and the international community has created large financial silos through which interventions have been funded. Creative work has been done by both sides. But with the expansion of antiretroviral therapy, the fiscal implications of HIV/AIDS are now too large to ignore. It is time for ministries of finance to be more directly involved in decisions on managing the liabilities to which countries are exposed, for the IMF to underscore the fiscal implications in all relevant cases, and for donor agencies to integrate HIV/AIDS funding needs into the general framework of development finance at the country level. ■
Paul Collier is Professor of Economics and Public Policy in the Blavatnik School of Government at the University of Oxford, where Richard Manning is a Senior Research Fellow. Olivier Sterck is a postdoctoral Fellow at the University of Oxford, at the Centre for the Study of African Economies.
This article is based on a paper (Collier, Sterck, and Manning, 2015) published as part of the work of RethinkHIV, a consortium of senior researchers, funded by the RUSH Foundation, who evaluate new evidence related to the costs, benefits, fiscal implications, and developmental impacts of HIV interventions in sub-Saharan Africa. The costing methodology in this article—and the conclusions drawn from applying it, about the relative cost-effectiveness of different policies—were originally developed by Markus Haacker.
References
Avenir Health (formerly Futures Institute), 2014, Spectrum Manual, Spectrum System of Policy Models (Glastonbury, Connecticut).
Collier, Paul, Olivier Sterck, and Richard Manning, 2015, “The Moral and Fiscal Implications of Antiretroviral Therapies for HIV in Africa,” CSAE Working Paper WPS/2015-05 (Oxford, United Kingdom: Centre for the Study of African Economies).
Haacker, Markus, and Elizabeth, Lule, 2011, The Fiscal Dimension of HIV/AIDS in Botswana, South Africa, Swaziland, and Uganda (Washington: World Bank).
Santelli, John S., Zoe R. Edelstein, Ying Wei, Sanyukta Mathur, Xiaoyu Song, and Ashley Schuyler, 2015, “Trends in HIV Acquisition, Risk Factors and Prevention Policies among Youth in Uganda, 1999–2011,” AIDS, Vol. 29, No. 2, pp. 211–19.
Schwartländer, Bernhard, John Stover, Timothy Hallett, and others, 2011, “Towards an Improved Investment Approach for an Effective Response to HIV/AIDS,” Lancet, Vol. 377, No. 9782, pp. 2031–41.
Stevens, Warren, Steve Kaye, and Tumani Corrah, 2004, “Antiretroviral Therapy in Africa,” BMJ, Vol. 328, No. 7434, p. 280.
UNAIDS, 2014, The Gap Report (Geneva).
World Health Organization (WHO), 2015, Guideline on When to Start Antiretroviral Therapy and on Pre-Exposure Prophylaxis for HIV (Geneva).


